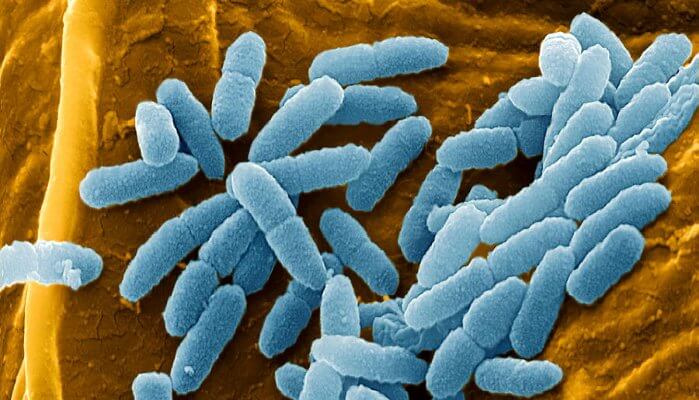
Susceptible strain of E. coli to different concentrations of fluoxetine. The SNAPPs were active against all bacterial species but were especially effective against Gram-negative bacteria like E. coli. certain antibiotic resistance genes are shared between the human gut microbiome are also present in multiple human pathogens. Antibiotic resistance in microorganisms has become an overwhelming problem nationally and globally. Their findings may help in the fight against bacterial infections, cancerous cells and allergies caused by allergens such as pollen. antibiotics that, can lead the survivors to pass on their antibiotic resistance genes.
As a result, the bacteria can not grow. Newswise-Bacteria-especially Gram-negative strains-are becoming increasingly resistant to current antibiotic drugs, and the development of new classes of antibiotics has slowed. Now new research indicates that such synergy may work even when bacteria become resistant to colistin, which is considered a treatment agent of last resort. It does so by a process called as the’ immune response ‘. All bacteria have a cell wall that protects the cell’s inner workings.
Microbes are single cell organisms that are further classified into Bacteria, Viruses, Eukaryotes, and Archaea. And now researchers have made a breakthrough. In a study published in the journal mBio on Tuesday, the researchers describe a system they call BacCapSeq, which they claim uses 4.2 million genetic probes to detect the signature DNA of all 307 kinds of pathogenic bacteria. The results showed that cellulose was detected in 14.8 percent of all the UTI samples. Scientists have traditionally believed that combining more than two drugs to fight harmful bacteria would yield diminishing returns.
“There is a tradition of using just one drug, maybe two”, said pamela yeh, one of the study’s senior authors of the paper. In reality, however rare, when traces of intact protein are absorbed. The results were reported in the journal Oncogene. With this breakthrough, we can use synthetic T cells to engineer more efficient drug carriers and understand the behavior of immune cells. The findings were published today in the journal Cell Reports. The researchers also tested their ability to fight infections.
Seven of the peptides were found to have antimicrobial activity against Pseudomonas aeruginosa as well as Staphylococcus aureus whereas the 8th peptide showed antimicrobial activity only towards P. aeruginosa. Scientists hoping to harness these peptides as potential antibiotics have now discovered that other peptides in the human body can also have potent antimicrobial effects, expanding the pool of new antibiotic candidates. Antibiotic resistant bacteria are “sleeper cells” which can survive doses of antibiotics and lie resting in a dormant state, but have the ability to “wake up” and re-infect, research has found. Antibiotic resistance is one of the most pressing public health challenges and threatens the ability to effectively fight infectious diseases including pneumonia and tuberculosis. And that usually has unwanted side effects.
Out of the many amino acids available to them, the scientists chose lysine and valine. The SNAPPs may also trigger the cellular processes that induce apoptosis, or cell suicide. In the new study, researchers were able to make as many as 100 billion red blood cells-enough to fill two or three collection tubes-from a single plate of embryonic stem cells. Today, there are several ways of detecting cancer cells in blood. What keeps bacteria and archaea different from those of human cells are the absence of nuclei with DNA stored in it. Most gut bacteria live in a harmless relationship with the human host, so may not be an immediate threat to human health.
“To our knowledge this was the first time anyone had shown hospital bacteria becoming tolerant to alcohols”, says Timothy Stinear, a coauthor of the study and a researcher at the University of Melbourne’s Doherty Institute for Infection and Immunity. It has also hurts your body’s ability to fight off yeast infections by making your immune system less effective. This showed that these peptides can act synergistically with FLC. However, such studies have been mainly developed in the area of human pathogens. And much like a typical antibiotic, the bigger dose of fluoxetine the bacteria got, the quicker the surviving bacteria developed resistance.
The bacteria that lived through the fluoxetine bath were quick to develop mutations against the widely used antibiotics chloramphenicol, amoxicillin, and tetracycline, they found. This resistance was also seen against other antibiotics in the same drug class. Salmonella Typhimurium is disease-causing bacteria predominately found in the intestine. But every so often bacteria make it through. “While people may have experienced gastrointestinal issues because of Salmonella, these bacteria can be drug resistant and in some cases, become difficult to treat”, said Coombes. “Many bacteria produce AmpC b-lactamase only when b-lactam antibiotics are present, and this is controlled by a sensory’ on switch’ molecule found inside the bacteria”, Associate Professor Stubbs said. “The UWA-led research team has developed a compound that can stop switching on’ of the AmpC enzyme. The researchers found the same mechanism active in bifidobacteria too.
The combinations were effective because individual medications have different means of targeting E. coli. “That is the primary goal, but we will also be looking at the possibility of developing new drugs against infections in the eyes and various internal organs. For this theoretical work a specific bacterial strain ( E. coli ) was used, where the proteins on the bacterial surface are engineered to bind with the virus upon contact. Haynes and colleagues, including lead author Todd Bradley, Ph. D., designed the study to analyze the molecular differences between HIV-infected people who make bnAbs, and those who don’t.